X-rays are produced as a result. History of discovery and applications of X-rays
Modern medical diagnostics and treatment of certain diseases cannot be imagined without devices that use the properties of X-rays. The discovery of X-rays occurred more than 100 years ago, but even now work continues on the creation of new methods and apparatus to minimize the negative effect of radiation on the human body.
Who and how discovered X-rays
Under natural conditions, the flux of X-rays is rare and is emitted only by certain radioactive isotopes. x-ray radiation or X-rays were discovered only in 1895 by the German scientist Wilhelm Röntgen. This discovery happened by chance, during an experiment to study the behavior of light rays under conditions approaching vacuum. The experiment involved a cathode gas discharge tube with reduced pressure and a fluorescent screen, which each time began to glow at the moment when the tube began to act.
Interested in a strange effect, Roentgen conducted a series of studies showing that the resulting radiation, invisible to the eye, is able to penetrate various obstacles: paper, wood, glass, some metals, and even through the human body. Despite the lack of understanding of the very nature of what is happening, whether such a phenomenon is caused by the generation of a stream of unknown particles or waves, the following pattern was noted - radiation easily passes through the soft tissues of the body, and much harder through solid living tissues and inanimate substances.
Roentgen was not the first to study this phenomenon. In the middle of the 19th century, Frenchman Antoine Mason and Englishman William Crookes studied similar possibilities. However, it was Roentgen who first invented the cathode tube and an indicator that could be used in medicine. He was the first to publish a scientific work, which brought him the title of the first Nobel laureate among physicists.
In 1901, a fruitful collaboration began between the three scientists, who became the founding fathers of radiology and radiology.

X-ray properties
X-rays are an integral part of the general spectrum of electromagnetic radiation. The wavelength is between gamma and ultraviolet rays. X-rays have all the usual wave properties:
- diffraction;
- refraction;
- interference;
- propagation speed (it is equal to light).
To artificially generate an X-ray flux, special devices are used - X-ray tubes. X-ray radiation arises from the contact of fast tungsten electrons with substances evaporating from a hot anode. Against the background of interaction, short-length electromagnetic waves arise, which are in the spectrum from 100 to 0.01 nm and in the energy range of 100-0.1 MeV. If the wavelength of the rays is less than 0.2 nm - this is hard radiation, if the wavelength is greater than the specified value, they are called soft x-rays.
It is significant that the kinetic energy arising from the contact of electrons and the anode substance is 99% converted into heat energy and only 1% is X-rays.
X-ray radiation - bremsstrahlung and characteristic
X-radiation is a superposition of two types of rays - bremsstrahlung and characteristic. They are generated in the handset simultaneously. Therefore, X-ray irradiation and the characteristic of each specific X-ray tube - the spectrum of its radiation, depends on these indicators, and represents their superposition.
Bremsstrahlung or continuous X-rays are the result of deceleration of electrons evaporating from a tungsten filament.
Characteristic or line X-rays are formed at the moment of rearrangement of the atoms of the substance of the anode of the X-ray tube. The wavelength of the characteristic rays directly depends on the atomic number of the chemical element used to make the anode of the tube.
The listed properties of X-rays allow them to be used in practice:
- invisible to the ordinary eye;
- high penetrating ability through living tissues and inanimate materials that do not transmit visible light;
- ionization effect on molecular structures.
Principles of X-ray Imaging
The property of x-rays on which imaging is based is the ability to either decompose or cause some substances to glow.
X-ray irradiation causes a fluorescent glow in cadmium and zinc sulfides - green, and in calcium tungstate - blue. This property is used in the technique of medical X-ray transillumination, and also increases the functionality of X-ray screens.
The photochemical effect of X-rays on light-sensitive silver halide materials (illumination) makes it possible to carry out diagnostics - to take X-ray images. This property is also used in measuring the amount of the total dose that laboratory assistants receive in X-ray rooms. Wearable dosimeters have special sensitive tapes and indicators. The ionizing effect of X-ray radiation makes it possible to determine the qualitative characteristics of the obtained X-rays.
A single exposure to conventional X-rays increases the risk of cancer by only 0.001%.
Areas where X-rays are used
The use of X-rays is acceptable in the following industries:
- Safety. Fixed and portable devices for detecting dangerous and prohibited items at airports, customs or in crowded places.
- Chemical industry, metallurgy, archeology, architecture, construction, restoration work - to detect defects and conduct chemical analysis of substances.
- Astronomy. It helps to observe cosmic bodies and phenomena with the help of X-ray telescopes.
- military industry. For the development of laser weapons.
The main application of X-rays is in the medical field. Today, the section of medical radiology includes: radiodiagnostics, radiotherapy (X-ray therapy), radiosurgery. Medical universities produce highly specialized specialists - radiologists.
X-Radiation - harm and benefit, effects on the body
The high penetrating power and ionizing effect of X-rays can cause a change in the structure of the DNA of the cell, therefore it is dangerous for humans. The harm from X-ray radiation is directly proportional to the received radiation dose. Different organs respond to irradiation to varying degrees. The most susceptible include:
- bone marrow and bone tissue;
- lens of the eye;
- thyroid;
- mammary and sex glands;
- lung tissue.
Uncontrolled use of X-ray radiation can cause reversible and irreversible pathologies.
Consequences of X-ray exposure:
- damage to the bone marrow and the occurrence of pathologies of the hematopoietic system - erythrocytopenia, thrombocytopenia, leukemia;
- damage to the lens, with the subsequent development of cataracts;
- cellular mutations that are inherited;
- development of oncological diseases;
- getting radiation burns;
- development of radiation sickness.
Important! Unlike radioactive substances, X-rays do not accumulate in the tissues of the body, which means that there is no need to remove X-rays from the body. The harmful effect of X-rays ends when the medical device is turned off.
The use of X-rays in medicine is permissible not only for diagnostic (traumatology, dentistry), but also for therapeutic purposes:
- from x-rays in small doses, the metabolism in living cells and tissues is stimulated;
- certain limiting doses are used for the treatment of oncological and benign neoplasms.

Methods for diagnosing pathologies using X-rays
Radiodiagnostics includes the following methods:
- Fluoroscopy is a study in which an image is obtained on a fluorescent screen in real time. Along with the classical real-time imaging of a body part, today there are X-ray television transillumination technologies - the image is transferred from a fluorescent screen to a television monitor located in another room. Several digital methods have been developed for processing the resulting image, followed by transferring it from the screen to paper.
- Fluorography is the cheapest method for examining the chest organs, which consists in making a small picture of 7x7 cm. Despite the possibility of error, it is the only way to conduct a mass annual examination of the population. The method is not dangerous and does not require the withdrawal of the received radiation dose from the body.
- Radiography - obtaining a summary image on film or paper to clarify the shape of an organ, its position or tone. Can be used to assess peristalsis and the condition of the mucous membranes. If there is a choice, then among modern X-ray devices, preference should be given neither to digital devices, where the x-ray flux can be higher than that of old devices, but to low-dose X-ray devices with direct flat semiconductor detectors. They allow you to reduce the load on the body by 4 times.
- Computed X-ray tomography is a technique that uses x-rays to obtain the required number of images of sections of a selected organ. Among the many varieties of modern CT devices, low-dose high-resolution CT scanners are used for a series of repeated studies.

Radiotherapy
X-ray therapy refers to local treatment methods. Most often, the method is used to destroy cancer cells. Since the effect of exposure is comparable to surgical removal, this treatment method is often called radiosurgery.
Today, x-ray treatment is carried out in the following ways:
- External (proton therapy) - the radiation beam enters the patient's body from the outside.
- Internal (brachytherapy) - the use of radioactive capsules by implanting them into the body, with the placement closer to the cancerous tumor. The disadvantage of this method of treatment is that until the capsule is removed from the body, the patient needs to be isolated.
These methods are gentle, and their use is preferable to chemotherapy in some cases. Such popularity is due to the fact that the rays do not accumulate and do not require removal from the body, they have a selective effect, without affecting other cells and tissues.
Safe X-ray exposure rate
This indicator of the norm of permissible annual exposure has its own name - a genetically significant equivalent dose (GED). There are no clear quantitative values for this indicator.
- This indicator depends on the age and desire of the patient to have children in the future.
- It depends on which organs were examined or treated.
- The GZD is affected by the level of natural radioactive background of the region where a person lives.
Today, the following average GZD standards are in force:
- the level of exposure from all sources, with the exception of medical ones, and without taking into account the natural radiation background - 167 mRem per year;
- the norm for an annual medical examination is not more than 100 mRem per year;
- the total safe value is 392 mRem per year.
X-ray radiation does not require excretion from the body, and is dangerous only in case of intense and prolonged exposure. Modern medical equipment uses low-energy radiation of short duration, so its use is considered relatively harmless.
In 1895, the German physicist W. Roentgen discovered a new, previously unknown type of electromagnetic radiation, which was named X-ray in honor of its discoverer. W. Roentgen became the author of his discovery at the age of 50, holding the post of rector of the University of Würzburg and having a reputation as one of the best experimenters of his time. One of the first to find a technical application for Roentgen's discovery was the American Edison. He created a handy demonstration apparatus and already in May 1896 organized an X-ray exhibition in New York, where visitors could look at their own hand on a luminous screen. After Edison's assistant died from the severe burns he received from constant demonstrations, the inventor stopped further experiments with X-rays.
X-ray radiation began to be used in medicine due to its high penetrating power. Initially, X-rays were used to examine bone fractures and locate foreign bodies in the human body. Currently, there are several methods based on X-rays. But these methods have their drawbacks: radiation can cause deep damage to the skin. Appearing ulcers often turned into cancer. In many cases, fingers or hands had to be amputated. Fluoroscopy(synonymous with translucence) is one of the main methods of X-ray examination, which consists in obtaining a planar positive image of the object under study on a translucent (fluorescent) screen. During fluoroscopy, the subject is between a translucent screen and an x-ray tube. On modern X-ray translucent screens, the image appears at the moment the X-ray tube is turned on and disappears immediately after it is turned off. Fluoroscopy makes it possible to study the function of the organ - heart pulsation, respiratory movements of the ribs, lungs, diaphragm, peristalsis of the digestive tract, etc. Fluoroscopy is used in the treatment of diseases of the stomach, gastrointestinal tract, duodenum, diseases of the liver, gallbladder and biliary tract. At the same time, the medical probe and manipulators are inserted without tissue damage, and the actions during the operation are controlled by fluoroscopy and are visible on the monitor.
Radiography - method of X-ray diagnostics with the registration of a fixed image on a photosensitive material - special. photographic film (X-ray film) or photographic paper with subsequent photo processing; With digital radiography, the image is fixed in the computer's memory. It is performed on X-ray diagnostic devices - stationary, installed in specially equipped X-ray rooms, or mobile and portable - at the patient's bedside or in the operating room. On radiographs, the elements of the structures of various organs are displayed much more clearly than on a fluorescent screen. Radiography is performed in order to detect and prevent various diseases, its main goal is to help doctors of various specialties correctly and quickly make a diagnosis. An x-ray image captures the state of an organ or tissue only at the time of exposure. However, a single radiograph captures only anatomical changes at a certain moment, it gives the statics of the process; through a series of radiographs taken at certain intervals, it is possible to study the dynamics of the process, that is, functional changes. Tomography. The word tomography can be translated from Greek as slice image. This means that the purpose of tomography is to obtain a layered image of the internal structure of the object of study. Computed tomography is characterized by high resolution, which makes it possible to distinguish subtle changes in soft tissues. CT allows to detect such pathological processes that cannot be detected by other methods. In addition, the use of CT makes it possible to reduce the dose of X-ray radiation received by patients during the diagnostic process.
Fluorography- a diagnostic method that allows you to get an image of organs and tissues, was developed at the end of the 20th century, a year after X-rays were discovered. In the pictures you can see sclerosis, fibrosis, foreign objects, neoplasms, inflammations that have a developed degree, the presence of gases and infiltrate in the cavities, abscesses, cysts, and so on. Most often, a chest x-ray is performed, which allows to detect tuberculosis, a malignant tumor in the lungs or chest, and other pathologies.
X-ray therapy- This is a modern method with which the treatment of certain pathologies of the joints is performed. The main directions of treatment of orthopedic diseases by this method are: Chronic. Inflammatory processes of the joints (arthritis, polyarthritis); Degenerative (osteoarthritis, osteochondrosis, deforming spondylosis). The purpose of radiotherapy is the inhibition of the vital activity of cells of pathologically altered tissues or their complete destruction. In non-tumor diseases, X-ray therapy is aimed at suppressing the inflammatory reaction, inhibiting proliferative processes, reducing pain sensitivity and secretory activity of the glands. It should be borne in mind that the sex glands, hematopoietic organs, leukocytes, and malignant tumor cells are most sensitive to X-rays. The radiation dose in each case is determined individually.
For the discovery of X-rays, Roentgen was awarded the first Nobel Prize in Physics in 1901, and the Nobel Committee emphasized the practical importance of his discovery.
Thus, X-rays are invisible electromagnetic radiation with a wavelength of 105 - 102 nm. X-rays can penetrate some materials that are opaque to visible light. They are emitted during the deceleration of fast electrons in matter (continuous spectrum) and during transitions of electrons from the outer electron shells of the atom to the inner ones (linear spectrum). Sources of X-ray radiation are: X-ray tube, some radioactive isotopes, accelerators and accumulators of electrons (synchrotron radiation). Receivers - film, luminescent screens, nuclear radiation detectors. X-rays are used in X-ray diffraction analysis, medicine, flaw detection, X-ray spectral analysis, etc.
Radiology is a branch of radiology that studies the effects of X-ray radiation on the body of animals and humans arising from this disease, their treatment and prevention, as well as methods for diagnosing various pathologies using X-rays (X-ray diagnostics). A typical X-ray diagnostic apparatus includes a power supply (transformers), a high-voltage rectifier that converts alternating current electrical network in permanent, control panel, tripod and x-ray tube.
X-rays are a type of electromagnetic oscillations that are formed in an X-ray tube during a sharp deceleration of accelerated electrons at the moment of their collision with the atoms of the anode substance. At present, the point of view is generally accepted that X-rays, by their physical nature, are one of the types of radiant energy, the spectrum of which also includes radio waves, infrared rays, visible light, ultraviolet rays and gamma rays of radioactive elements. X-ray radiation can be characterized as a collection of its smallest particles - quanta or photons.
Rice. 1 - mobile x-ray machine:
A - x-ray tube;
B - power supply;
B - adjustable tripod.
 Rice. 2 - X-ray machine control panel (mechanical - on the left and electronic - on the right):
Rice. 2 - X-ray machine control panel (mechanical - on the left and electronic - on the right): A - panel for adjusting exposure and hardness;
B - feed button high voltage.
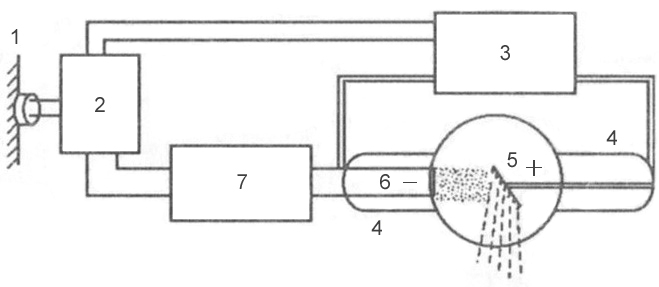 Rice. 3 is a block diagram of a typical x-ray machine
Rice. 3 is a block diagram of a typical x-ray machine 1 - network;
2 - autotransformer;
3 - step-up transformer;
4 - x-ray tube;
5 - anode;
6 - cathode;
7 - step-down transformer.
Mechanism of X-ray generation
X-rays are formed at the moment of collision of a stream of accelerated electrons with the anode material. When electrons interact with a target, 99% of their kinetic energy is converted into thermal energy and only 1% - in x-rays.
An X-ray tube consists of a glass container in which 2 electrodes are soldered: a cathode and an anode. Air is pumped out of the glass cylinder: the movement of electrons from the cathode to the anode is possible only under conditions of relative vacuum (10 -7 -10 -8 mm Hg). On the cathode there is a filament, which is a tightly twisted tungsten filament. When an electric current is applied to the filament, electron emission occurs, in which electrons are separated from the spiral and form an electron cloud near the cathode. This cloud is concentrated at the focusing cup of the cathode, which sets the direction of electron movement. Cup - a small depression in the cathode. The anode, in turn, contains a tungsten metal plate on which the electrons are focused - this is the site of the formation of x-rays.
Rice. 4 - X-ray tube device: A - cathode; 
B - anode;
B - tungsten filament;
G - focusing cup of the cathode;
D - stream of accelerated electrons;
E - tungsten target;
G - glass flask;
З - a window from beryllium;
And - formed x-rays;
K - aluminum filter.
2 transformers are connected to the electron tube: step-down and step-up. A step-down transformer heats the tungsten filament with a low voltage (5-15 volts), resulting in electron emission. A step-up, or high-voltage, transformer goes directly to the cathode and anode, which are supplied with a voltage of 20–140 kilovolts. Both transformers are placed in the high-voltage block of the X-ray machine, which is filled with transformer oil, which provides cooling of the transformers and their reliable insulation.
After an electron cloud has formed with the help of a step-down transformer, the step-up transformer is turned on, and high-voltage voltage is applied to both poles of the electrical circuit: a positive pulse to the anode, and a negative pulse to the cathode. Negatively charged electrons are repelled from a negatively charged cathode and tend to a positively charged anode - due to such a potential difference, a high speed of movement is achieved - 100 thousand km / s. At this speed, electrons bombard the tungsten plate of the anode, shorting out electrical circuit, resulting in X-rays and thermal energy.
X-ray radiation is subdivided into bremsstrahlung and characteristic. Bremsstrahlung occurs due to a sharp deceleration of the speed of electrons emitted by a tungsten filament. Characteristic radiation occurs at the moment of rearrangement of the electron shells of atoms. Both of these types are formed in an X-ray tube at the moment of collision of accelerated electrons with atoms of the anode material. The emission spectrum of an X-ray tube is a superposition of bremsstrahlung and characteristic X-rays.
 Rice. 5 - the principle of the formation of bremsstrahlung X-rays.
Rice. 5 - the principle of the formation of bremsstrahlung X-rays.
 Rice. 6 - the principle of formation of the characteristic x-ray radiation.
Rice. 6 - the principle of formation of the characteristic x-ray radiation.
Basic properties of X-rays
- X-rays are invisible to visual perception.
- X-ray radiation has a great penetrating power through the organs and tissues of a living organism, as well as dense structures of inanimate nature, which do not transmit visible light rays.
- X-rays cause certain chemical compounds to glow, called fluorescence.
- Zinc and cadmium sulfides fluoresce yellow-green,
- Crystals of calcium tungstate - violet-blue.
Scale of electromagnetic oscillations
X-rays have a specific wavelength and frequency of oscillation. Wavelength (λ) and oscillation frequency (ν) are related by the relationship: λ ν = c, where c is the speed of light, rounded to 300,000 km per second. The energy of X-rays is determined by the formula E = h ν, where h is Planck's constant, a universal constant equal to 6.626 10 -34 J⋅s. The wavelength of the rays (λ) is related to their energy (E) by the relation: λ = 12.4 / E.
X-ray radiation differs from other types of electromagnetic oscillations in wavelength (see table) and quantum energy. The shorter the wavelength, the higher its frequency, energy and penetrating power. The X-ray wavelength is in the range
. By changing the wavelength of X-ray radiation, it is possible to control its penetrating power. X-rays have a very short wavelength, but a high frequency of oscillation, so they are invisible to the human eye. Due to their enormous energy, quanta have a high penetrating power, which is one of the main properties that ensure the use of X-rays in medicine and other sciences.X-ray characteristics
Intensity- quantitative characteristic of x-ray radiation, which is expressed by the number of rays emitted by the tube per unit time. The intensity of X-rays is measured in milliamps. Comparing it with the intensity of visible light from ordinary lamp incandescent, we can draw an analogy: for example, a 20-watt lamp will shine with one intensity, or power, and a 200-watt lamp will shine with another, while the quality of the light itself (its spectrum) is the same. The intensity of X-ray radiation is, in fact, its quantity. Each electron creates one or more radiation quanta on the anode, therefore, the number of X-rays during exposure of the object is regulated by changing the number of electrons tending to the anode and the number of interactions of electrons with atoms of the tungsten target, which can be done in two ways:
- By changing the degree of incandescence of the cathode spiral using a step-down transformer (the number of electrons produced during emission will depend on how hot the tungsten spiral is, and the number of radiation quanta will depend on the number of electrons);
- By changing the value of the high voltage supplied by the step-up transformer to the poles of the tube - the cathode and the anode (the higher the voltage is applied to the poles of the tube, the more kinetic energy the electrons receive, which, due to their energy, can interact with several atoms of the anode substance in turn - see Fig. rice. 5; electrons with low energy will be able to enter into a smaller number of interactions).
The X-ray intensity (anode current) multiplied by the exposure (tube time) corresponds to the X-ray exposure, which is measured in mAs (milliamps per second). Exposure is a parameter that, like intensity, characterizes the amount of rays emitted by an x-ray tube. The only difference is that the exposure also takes into account the operating time of the tube (for example, if the tube works for 0.01 sec, then the number of rays will be one, and if 0.02 sec, then the number of rays will be different - twice more). The radiation exposure is set by the radiologist on the control panel of the X-ray machine, depending on the type of examination, the size of the object under study and the diagnostic task.
Rigidity- qualitative characteristic of x-ray radiation. It is measured by the high voltage on the tube - in kilovolts. Determines the penetrating power of x-rays. It is regulated by the high voltage supplied to the X-ray tube by a step-up transformer. The higher the potential difference is created on the electrodes of the tube, the more force the electrons repel from the cathode and rush to the anode, and the stronger their collision with the anode. The stronger their collision, the shorter the wavelength of the resulting X-ray radiation and the higher the penetrating power of this wave (or the hardness of the radiation, which, like the intensity, is regulated on the control panel by the voltage parameter on the tube - kilovoltage).
λ - wavelength;  Rice. 7 - Dependence of the wavelength on the energy of the wave:
Rice. 7 - Dependence of the wavelength on the energy of the wave:
E - wave energy  Rice. 8 - The ratio of the voltage on the X-ray tube and the wavelength of the resulting X-ray radiation:
Rice. 8 - The ratio of the voltage on the X-ray tube and the wavelength of the resulting X-ray radiation:
Classification of x-ray tubes
- By appointment
- Diagnostic
- Therapeutic
- For structural analysis
- For transillumination
- By design
- By focus
- Single-focus (one spiral on the cathode, and one focal spot on the anode)
- Bifocal (two spirals of different sizes on the cathode, and two focal spots on the anode)
- By type of anode
- Stationary (fixed)
- Rotating
X-rays are used not only for radiodiagnostic purposes, but also for therapeutic purposes. As noted above, the ability of X-ray radiation to suppress the growth of tumor cells makes it possible to use it in radiation therapy of oncological diseases. Apart from medical field applications, X-ray radiation has found wide application in the engineering and technical field, materials science, crystallography, chemistry and biochemistry: for example, it is possible to identify structural defects in various products (rails, welds, etc.) using X-ray radiation. The type of such research is called defectoscopy. And at airports, railway stations and other crowded places, X-ray television introscopes are actively used to scan hand luggage and luggage for security purposes.
Depending on the type of anode, X-ray tubes differ in design. Due to the fact that 99% of the kinetic energy of the electrons is converted into thermal energy, during the operation of the tube, the anode is significantly heated - the sensitive tungsten target often burns out. The anode is cooled in modern x-ray tubes by rotating it. The rotating anode has the shape of a disk, which distributes heat evenly over its entire surface, preventing local overheating of the tungsten target.
The design of X-ray tubes also differs in focus. Focal spot - the section of the anode on which the working X-ray beam is generated. It is subdivided into the real focal spot and the effective focal spot ( rice. 12). Due to the angle of the anode, the effective focal spot is smaller than the real one. Different focal spot sizes are used depending on the size of the image area. The larger the image area, the wider the focal spot must be to cover the entire image area. However, a smaller focal spot produces better image clarity. Therefore, when producing small images, a short filament is used and the electrons are directed to a small area of the anode target, creating a smaller focal spot.
 Rice. 9 - x-ray tube with a stationary anode.
Rice. 9 - x-ray tube with a stationary anode.
 Rice. 10 - X-ray tube with a rotating anode.
Rice. 10 - X-ray tube with a rotating anode.
 Rice. 11 - X-ray tube device with a rotating anode.
Rice. 11 - X-ray tube device with a rotating anode.
 Rice. 12 is a diagram of the formation of a real and effective focal spot.
Rice. 12 is a diagram of the formation of a real and effective focal spot.
High penetrating ability - able to penetrate certain media. X-rays penetrate best through gaseous media (lung tissue), but poorly penetrate through substances with high electron density and large atomic mass (bones in humans).
Fluorescence - glow. In this case, the energy of X-rays is converted into the energy of visible light. Currently, the principle of fluorescence underlies the device of intensifying screens designed for additional illumination of X-ray film. This allows you to reduce the radiation load on the body of the patient under study.
Photochemical - the ability to induce various chemical reactions.
Ionizing ability - under the influence of X-rays, ionization of atoms occurs (decomposition of neutral molecules into positive and negative ions that make up an ion pair.
Biological - damage to cells. For the most part, it is due to the ionization of biologically significant structures (DNA, RNA, protein molecules, amino acids, water). Positive biological effects - antitumor, anti-inflammatory.
Beam tube device
X-rays are produced in an X-ray tube. An X-ray tube is a glass container with a vacuum inside. There are 2 electrodes - cathode and anode. The cathode is a thin tungsten spiral. The anode in the old tubes was a heavy copper rod, with a bevelled surface facing the cathode. On the beveled surface of the anode, a plate of refractory metal was soldered - the mirror of the anode (the anode is very hot during operation). In the center of the mirror is focus of x-ray tube This is where X-rays are produced. The smaller the focus value, the clearer the contours of the subject being shot are. Small focus is considered 1x1 mm, and even less.
In modern X-ray machines, electrodes are made from refractory metals. Typically, tubes with a rotating anode are used. During operation, the anode is rotated by a special device, and the electrons flying from the cathode fall into the optical focus. Due to the rotation of the anode, the position of the optical focus changes all the time, so such tubes are more durable and do not wear out for a long time.
How are x-rays obtained? First, the cathode filament is heated. To do this, using a step-down transformer, the voltage on the tube is reduced from 220 to 12-15V. The cathode filament heats up, the electrons in it begin to move faster, some of the electrons go beyond the filament and a cloud of free electrons forms around it. After that, a high voltage current is turned on, which is obtained using a step-up transformer. In diagnostic X-ray machines, high voltage current is used from 40 to 125 KV (1KV=1000V). The higher the voltage on the tube, the shorter the wavelength. When a high voltage is turned on, a large potential difference is obtained at the poles of the tube, the electrons “break off” from the cathode and rush to the anode at high speed (the tube is the simplest charged particle accelerator). Thanks to special devices, the electrons do not scatter to the sides, but fall into almost one point of the anode - the focus (focal spot) and are decelerated in the electric field of the anode atoms. When the electrons decelerate, electromagnetic waves arise, i.e. X-rays. Thanks to a special device (in old tubes - the bevel of the anode), x-rays are directed to the patient in the form of a divergent beam of rays, a "cone".
X-ray imaging
X-ray film is a layered structure, the main layer is a polyester composition up to 175 microns thick, coated with a photographic emulsion (silver iodide and bromide, gelatin).
Film development - silver is restored (where the rays passed through - blackening of the film area, where they lingered - lighter areas)
Fixer - washing out silver bromide from areas where the rays passed through and did not linger.
The device of a modern radiological room
1. The X-ray room itself, where the apparatus is located and the patients are examined. The area of the X-ray room must be at least 50 m2
2. Control room, where the control panel is located, with the help of which the X-ray laboratory assistant controls the entire operation of the device.
3. A photographic laboratory where cassettes are loaded with film, images are developed and fixed, they are washed and dried. A modern method of photo processing of medical X-ray films is the use of roller-type processors. In addition to undoubted convenience in work, processors provide high stability of the photo processing process. The time of a complete cycle from the moment the film enters the processing machine to the receipt of a dry X-ray pattern ("from dry to dry") does not exceed several minutes.
4. Doctor's office, where the radiologist analyzes and describes the radiographs taken.
Methods of protection for medical personnel and for patients from x-ray radiation
3 main protection methods: protection by shielding, distance and time.
1 .Shield protection:
X-rays are placed in the path of special devices made of materials that absorb x-rays well. It can be lead, concrete, barite concrete, etc. The walls, floor, ceiling in X-ray rooms are protected, made of materials that do not transmit rays into neighboring rooms. The doors are protected with lead material. The observation windows between the X-ray room and the control room are made of leaded glass. The x-ray tube is placed in a special protective casing that does not let x-rays through, and the rays are directed to the patient through a special "window". A tube is attached to the window, which limits the size of the x-ray beam. In addition, the X-ray machine diaphragm is installed at the exit of the rays from the tube. It consists of 2 pairs of plates perpendicular to each other. These plates can be moved and moved apart like curtains. In this way, the irradiation field can be increased or decreased. The larger the irradiation field, the greater the harm, therefore aperture is an important part of protection, especially in children. In addition, the doctor himself is irradiated less. And the quality of the pictures will be better. Another example of shielding is sewn up - those parts of the body of the subject that are not currently subject to shooting should be covered with sheets of lead rubber. There are also aprons, skirts, gloves made of special protective material.
2 .Protection by time:
The patient should be irradiated during x-ray examination for as little time as possible (hurry, but not to the detriment of diagnosis). In this sense, images give a lower radiation load than transillumination, because. very slow shutter speeds (time) are used in the pictures. Time protection is the main way to protect both the patient and the radiologist himself. When examining patients, the doctor, ceteris paribus, tries to choose a research method that takes less time, but not to the detriment of diagnosis. In this sense, fluoroscopy is more harmful, but, unfortunately, it is often impossible to do without fluoroscopy. So in the study of the esophagus, stomach, intestines, both methods are used. When choosing a research method, we are guided by the rule that the benefits of research should be greater than the harm. Sometimes, due to the fear of taking an extra picture, errors in diagnosis occur, treatment is incorrectly prescribed, which sometimes costs the patient's life. It is necessary to remember about the dangers of radiation, but do not be afraid of it, it is worse for the patient.
3 .Protection distance:
According to the quadratic law of light, the illumination of a given surface is inversely proportional to the square of the distance from the light source to the illuminated surface. In relation to X-ray examination, this means that the radiation dose is inversely proportional to the square of the distance from the focus of the X-ray tube to the patient (focal length). With an increase in the focal length by 2 times, the radiation dose decreases by 4 times, with an increase in the focal length by 3 times, the radiation dose decreases by 9 times.
A focal length of less than 35 cm is not allowed for fluoroscopy. The distance from the walls to the X-ray machine must be at least 2 m, otherwise secondary rays are formed that occur when the primary beam of rays hits the surrounding objects (walls, etc.). For the same reason, extra furniture is not allowed in X-ray rooms. Sometimes, when examining seriously ill patients, the personnel of the surgical and therapeutic departments help the patient stand behind the screen for transillumination and stand next to the patient during the examination, supporting him. As an exception, this is allowed. But the radiologist must make sure that the nurses and nurses helping the sick put on a protective apron and gloves and, if possible, do not stand close to the patient (protection by distance). If several patients came to the X-ray room, they are called to the procedural room by 1 person, i.e. There should only be 1 person at a time in the study.
Physical bases of radiography and fluorography. Their shortcomings and advantages. Advantages of digital over film.
Principles of radiography
For diagnostic radiography, it is advisable to take pictures in at least two projections. This is due to the fact that the radiograph is a flat image of a three-dimensional object. And as a result, the localization of the detected pathological focus can be established only with the help of 2 projections.
Imaging technique
The quality of the resulting X-ray image is determined by 3 main parameters. The voltage applied to the X-ray tube, the current strength and the operating time of the tube. Depending on the studied anatomical formations, and the weight and size data of the patient, these parameters can vary significantly. There are average values for different organs and tissues, but it should be borne in mind that the actual values will differ depending on the apparatus where the examination is performed and the patient who is being X-rayed. An individual table of values is compiled for each device. These values are not absolute and are adjusted as the study progresses. The quality of the images performed is largely dependent on the ability of the radiographer to adequately adapt the table of average values to a particular patient.
Image recording
The most common way to record an X-ray image is to fix it on an X-ray sensitive film and then develop it. Currently, there are also systems that provide digital data recording. Due to the high cost and complexity of manufacturing, this type of equipment is somewhat inferior to analog equipment in terms of prevalence.
X-ray film is placed in special devices - cassettes (they say - the cassette is loaded). The cassette protects the film from visible light; the latter, like x-rays, has the ability to reduce metallic silver from AgBr. Cassettes are made of a material that does not transmit light, but transmits x-rays. Inside the cassettes are intensifying screens, the film is laid between them; when taking a picture, not only the X-rays themselves fall on the film, but also the light from the screens (the screens are covered with fluorescent salt, so they glow and enhance the action of the X-rays). This allows you to reduce the radiation load on the patient by 10 times.
When taking a picture, x-rays are directed to the center of the object being photographed (centration). After shooting in a photo lab, the film is developed in special chemicals and fixed (fixed). The fact is that on those parts of the film that were not hit by x-rays during the shooting or there were few of them, silver was not restored, and if the film is not placed in a fixer (fixer) solution, then when examining the film, silver is restored under the influence of visible light. Sveta. The entire film will turn black and no image will be visible. When fixing (fixing), unreduced AgBr from the film goes into the fixer solution, so there is a lot of silver in the fixer, and these solutions are not poured out, but surrendered to X-ray centers.
A modern method of photo processing of medical X-ray films is the use of roller-type processors. In addition to undoubted convenience in work, processors provide high stability of the photo processing process. The time of a complete cycle from the moment the film enters the processing machine to the receipt of a dry X-ray pattern ("from dry to dry") does not exceed several minutes.
X-rays are an image made in black and white - a negative. Black - areas with low density (lungs, stomach gas bubble. White - with high density(bones).
Fluorography- The essence of FOG is that with it, an image of the chest is first obtained on a fluorescent screen, and then a picture is taken not of the patient himself, but of his image on the screen.
Fluorography gives a reduced image of the object. There are small frame (eg 24×24 mm or 35×35 mm) and large frame (eg 70×70 mm or 100×100 mm) techniques. The latter, in terms of diagnostic capabilities, approaches radiography. FOG is used for preventive examination of the population(hidden diseases such as cancer and tuberculosis are detected).
Both stationary and mobile fluorographic devices have been developed.
Currently, film fluorography is gradually being replaced by digital. Digital methods make it possible to simplify work with an image (an image can be displayed on a monitor screen, printed, transmitted over a network, stored in a medical database, etc.), reduce radiation exposure to the patient and reduce the cost of additional materials (film, developer for films).
There are two common methods of digital fluorography. The first technique, like conventional fluorography, uses photographing an image on a fluorescent screen, only a CCD matrix is used instead of an X-ray film. The second technique uses layer-by-layer transverse scanning of the chest with a fan-shaped X-ray beam with detection of the transmitted radiation by a linear detector (similar to a conventional paper document scanner, where the linear detector moves along a sheet of paper). The second method allows the use of much lower doses of radiation. Some drawback of the second method is the longer time for obtaining the image.
Comparative characteristics of the dose load in various studies.
A conventional film chest fluorogram provides the patient with an average individual radiation dose of 0.5 millisievert (mSv) per procedure (digital fluorogram - 0.05 mSv), while a film radiograph - 0.3 mSv per procedure (digital radiograph - 0 .03 mSv), and computed tomography of the chest - 11 mSv per procedure. Magnetic resonance imaging does not carry radiation exposure
Benefits of radiography
Wide availability of the method and ease of research.
Most studies do not require special patient preparation.
Relatively low cost of research.
The images can be used for consultation with another specialist or in another institution (unlike ultrasound images, where a second examination is necessary, since the images obtained are operator-dependent).
Static image - the complexity of assessing the function of the body.
The presence of ionizing radiation that can have a harmful effect on the patient.
The informativeness of classical radiography is much lower than such modern methods of medical imaging as CT, MRI, etc. Ordinary x-ray images reflect the projection layering of complex anatomical structures, that is, their summation x-ray shadow, in contrast to the layered series of images obtained by modern tomographic methods.
Without the use of contrast agents, radiography is not informative enough to analyze changes in soft tissues that differ little in density (for example, when studying abdominal organs).
Physical bases of roentgenoscopy. Disadvantages and advantages of the method
In modern conditions, the use of a fluorescent screen is not justified due to its low luminosity, which makes it necessary to conduct research in a well-darkened room and after a long adaptation of the researcher to the dark (10-15 minutes) to distinguish a low-intensity image.
Now fluorescent screens are used in the design of X-ray image intensifier, which increases the brightness (glow) of the primary image by about 5,000 times. With the help of an electron-optical converter, the image appears on the monitor screen, which significantly improves the quality of diagnostics, does not require darkening of the X-ray room.
Advantages of fluoroscopy
The main advantage over radiography is the fact of the study in real time. This allows you to evaluate not only the structure of the organ, but also its displacement, contractility or extensibility, the passage of a contrast agent, and fullness. The method also allows you to quickly assess the localization of some changes, due to the rotation of the object of study during transillumination (multi-projection study).
Fluoroscopy allows you to control the implementation of some instrumental procedures - catheter placement, angioplasty (see angiography), fistulography.
The resulting images can be placed on a regular CD or network storage.
With the advent of digital technologies, 3 main disadvantages inherent in traditional fluoroscopy have disappeared:
Relatively high radiation dose compared to radiography - modern low-dose devices have left this disadvantage in the past. The use of pulsed scan modes further reduces the dose load by up to 90%.
Low spatial resolution - on modern digital devices, the resolution in scopy mode is only slightly inferior to the resolution in radiographic mode. In this case, the ability to observe the functional state of individual organs (heart, lungs, stomach, intestines) "in dynamics" is of decisive importance.
The impossibility of documenting research - digital imaging technologies make it possible to save research materials, both frame-by-frame and as a video sequence.
Fluoroscopy is performed mainly in the X-ray diagnosis of diseases of the internal organs located in the abdominal and chest cavities, according to the plan that the radiologist draws up before the start of the study. Sometimes, the so-called survey fluoroscopy is used to recognize traumatic bone injuries, to clarify the area to be radiographed.
Contrast fluoroscopic examination
Artificial contrast greatly expands the possibilities of fluoroscopic examination of organs and systems where tissue densities are approximately the same (for example, abdomen, whose organs transmit X-rays to approximately the same extent and therefore have low contrast). This is achieved by introducing into the lumen of the stomach or intestines an aqueous suspension of barium sulfate, which does not dissolve in digestive juices, is not absorbed by the stomach or intestines and is excreted naturally in a completely unchanged form. The main advantage of barium suspension is that, passing through the esophagus, stomach and intestines, coats their inner walls and gives a complete picture of the nature of elevations, depressions and other features of their mucous membrane on the screen or film. The study of the internal relief of the esophagus, stomach and intestines contributes to the recognition of a number of diseases of these organs. With more tight filling, it is possible to determine the shape, size, position and function of the organ under study.
Mammography - the basics of the method, indications. Advantages of digital mammography over film.
Mammography- chapter medical diagnostics, engaged in non-invasive researchmammary gland, mainly female, which is carried out with the aim of:
1. prophylactic examination (screening) of healthy women to detect early, non-palpable forms of breast cancer;
2. differential diagnosis between cancer and benign dyshormonal hyperplasia (FAM) of the breast;
3. assessment of the growth of the primary tumor (single node or multicentric cancerous foci);
4.Dynamic dispensary monitoring of the state of the mammary glands after surgery.
The following methods of radiation diagnostics of breast cancer have been introduced into medical practice: mammography, ultrasound, computed tomography, magnetic resonance imaging, color and power Doppler, mammography-guided stereotaxic biopsy, and thermography.
X-ray mammography
Currently, in the world, in the vast majority of cases, X-ray projection mammography, film (analogue) or digital, is used to diagnose female breast cancer (BC).
The procedure takes no more than 10 minutes. For the shot, the chest should be fixed between two planks and slightly compressed. The picture is taken in two projections so that you can accurately determine the location of the neoplasm, if it is found. Because symmetry is one of the diagnostic factors, both breasts should always be examined.
MRI mammography
Complaints about retraction or bulging of any part of the gland
Discharge from the nipple, changing its shape
Soreness of the mammary gland, its swelling, resizing
As a preventive screening method, mammography is prescribed for all women aged 40 and older, or women who are at risk.
Benign breast tumors (particularly fibroadenoma)
Inflammatory processes (mastitis)
Mastopathy
Tumors of the genital organs
Diseases of the endocrine glands (thyroid, pancreas)
Infertility
Obesity
History of breast surgery
Advantages of digital mammography over film:
Reduction of dose loads during X-ray studies;
Improving the efficiency of research, allowing to identify previously inaccessible pathological processes (possibility of digital computer image processing);
Possibilities of using telecommunication networks for transmitting images for the purpose of remote consultation;
Achievement of economic effect during mass research.
X-ray radiation, from the point of view of physics, is electromagnetic radiation, the wavelength of which varies in the range from 0.001 to 50 nanometers. It was discovered in 1895 by the German physicist W.K. Roentgen.
By nature, these rays are related to solar ultraviolet. Radio waves are the longest in the spectrum. They are followed by infrared light, which our eyes do not perceive, but we feel it as heat. Next come the rays from red to purple. Then - ultraviolet (A, B and C). And right behind it are x-rays and gamma rays.
X-ray can be obtained in two ways: by deceleration in the matter of charged particles passing through it and by the transition of electrons from the upper layers to the internal ones when energy is released.
Unlike visible light, these rays are very long, so they are able to penetrate opaque materials without being reflected, refracted, or accumulated in them.
Bremsstrahlung is easier to obtain. Charged particles emit electromagnetic radiation when braking. The greater the acceleration of these particles and, consequently, the sharper the deceleration, the more X-rays are produced, and the wavelength becomes shorter. In most cases, in practice, they resort to the generation of rays in the process of deceleration of electrons in solids. This allows you to control the source of this radiation, avoiding the danger of radiation exposure, because when the source is turned off, the X-ray emission completely disappears.
The most common source of such radiation - The radiation emitted by it is inhomogeneous. It contains both soft (long-wave) and hard (short-wave) radiation. Soft is characterized by being completely absorbed human body, therefore, such X-ray radiation brings harm twice as much as hard. With excessive electromagnetic radiation in the tissues of the human body, ionization can damage cells and DNA.
The tube is with two electrodes - a negative cathode and a positive anode. When the cathode is heated, electrons evaporate from it, then they are accelerated in an electric field. Colliding with the solid matter of the anodes, they begin deceleration, which is accompanied by the emission of electromagnetic radiation.
X-ray radiation, the properties of which are widely used in medicine, is based on obtaining a shadow image of the object under study on a sensitive screen. If the diagnosed organ is illuminated with a beam of rays parallel to each other, then the projection of shadows from this organ will be transmitted without distortion (proportionally). In practice, the radiation source is more like a point source, so it is located at a distance from the person and from the screen.
To receive a person is placed between the x-ray tube and the screen or film, acting as radiation receivers. As a result of irradiation, bone and other dense tissues appear in the image as clear shadows, look more contrast against the background of less expressive areas that transmit tissues with less absorption. On x-rays, a person becomes "translucent".
As X-rays propagate, they can be scattered and absorbed. Before absorption, the rays can travel hundreds of meters in the air. In dense matter, they are absorbed much faster. Human biological tissues are heterogeneous, so their absorption of rays depends on the density of the tissue of the organs. absorbs rays faster than soft tissues, because it contains substances that have large atomic numbers. Photons (individual particles of rays) are absorbed by different tissues of the human body in different ways, which makes it possible to obtain a contrast image using X-rays.